In patients who only have partial erections or who either do not respond to other treatments or prefer not to use them, a vacuum device maybe useful. The device consists of a plastic cylinder connected to a pump and a constriction ring. A vacuum pump uses either manual or battery power to create suction around the penis and bring blood into it; a constriction device is then released around the base of the penis to keep blood in the penis and maintain the erection. A vacuum device can be used safely for up to 30 minutes, which is when the constriction device should be removed. The advantage of such a device is it is relatively inexpensive, easy to use and avoids drug interactions and side effects. Side effects may include temporary penile numbness, trapping the ejaculate and some bruising.
Penile prosthesis
For men with erectile dysfunction who have failed or cannot tolerate other treatments, a penile prosthesis offers an effective, but more invasive alternative. Prostheses come in either a semi-rigid form or as an inflatable device. Most men prefer the placement of the inflatable penile prosthesis.
The placement of the prosthesis within the penis requires the use of an anesthetic. A skin incision is made either at the junction of the penis and scrotum, or just above the penis, depending on which prosthesis and technique is used. The spongy tissue of the penis is exposed and dilated; the prosthesis is then sized and the proper device is then placed. The inflatable device — a pump that contains the inflation and deflation mechanism — is placed in the scrotum. The patient can control his erection at will by pushing a button under the skin. Although placement of the prosthesis requires a surgical procedure, patient and partner satisfaction rates are as high as 85 percent. Full penile length might not be restored to the patient’s natural erect status. Rare side effects include infection, pain and device malfunction or failure. As the nerves that control sensation are not injured, the penile sensation and the ability to have an orgasm should be maintained.
Psychological Causes of Impotence
Common causes of psychogenic impotence include depression and performance anxiety. Depression is associated with decreased energy, interest and decreased libido or desire. Performance anxiety, work stress or strained personal relationships can affect erectile function in both conscious and subconscious ways.
Neurogenic Impotence
Penile erection depends on an intact nervous system so any injury to the nervous system involved in erections may cause impotence. Diseases such as Parkinson’s disease, Alzheimer’s disease, stroke or head injury can lead to impotence by affecting the libido, or by preventing the initiation of the nerve impulses responsible for erections. Patients with spinal cord injuries will have decreased erections related to the extent of the injury. Patients who have undergone pelvic surgery such as radical prostatectomy, cystectomy or colectomy may have injury to the cavernous nerves that control erection. Long-standing diabetes may affect some nerves as well as causing impotence.
Hormonal Causes of Impotence
Diseases and conditions that decrease circulating testosterone in the body, such as castration or hormonal therapy used to treat prostate cancer, will decrease libido and impair erections.
Vascular Causes of Impotence
Diseases such as high blood pressure, high triglyceride and cholesterol levels in the blood, cigarette smoking and diabetes mellitus, and treatments such as pelvic irradiation to treat prostate, bladder and rectal cancers, may damage blood vessels to the penis over time. There is strong epidemiological association between heart disease, hypertension, low levels of high-density lipoproteins (HDL) and impotence. Patients with Peyronnie’s disease which causes curvature of the penis, trauma, diabetes or old age may have damage to the spongy tissue of the penis, causing the veins to be more “leaky,” which can lead to impotence.
Drugs and Impotence
Certain anti-depressants or anti-psychotics have been associated with impotence, especially those drugs that regulate serotonin, noradrenaline and dopamine. These include Prozac, Zoloft and Paxil. Beta-blockers and thiazide agents used to treat hypertension are associated with impotence. Cimetidine, a drug to treat acid reflux disease; chronic alcoholism; estrogens and drugs with anti-androgen action such as ketoconazole, and spironolactone can cause impotence, decreased libido and male breast enlargement. Even moderate alcohol intake may have an effect.
Aging and diseases which cause impotence
Aging, even in healthy men causes a progressive decline in sexual function. Medical studies have discovered that as men age, there is a decrease in turgidity, or “stiffness,” of erections as well as a decrease in the force and volume of ejaculation. Also, with normal aging, there is an increase in the length of time required between erections after orgasm, called the refractory period. Further, the sensitivity to touch decreases over time as do serum testosterone levels, with an associated decrease in desire. Studies indicate that half of all men with diabetes will eventually develop impotence. In addition, those with liver cirrhosis, chronic renal failure or coronary artery disease have a high incidence of impotence.
Normal male sexual function is a constellation of processes: sexual desire or libido, the erection when the penis becomes firm, release of semen (ejaculation) and orgasm. Erectile dysfunction — commonly known as impotence — is defined as the inability to achieve or maintain an erection that is sufficient for satisfactory sexual activity. However, almost all men who have impotence can overcome it.
– Sexual desire, the release and expulsion of semen — emission and ejaculation — and the ability to have an orgasm occur via separate, distinct physical mechanisms. Due to a variety of reasons they can be dissociated from one another. For example, orgasm and ejaculation can occur without erection.
– Sexual desire or libido is determined mainly by the amount of testosterone in the body. As men get older the amount of testosterone that circulates slowly declines, decreasing libido. A decrease in libido also may result from depression and various medical problems that affect overall mental and physical well being.
– Ejaculation, the expulsion of semen during sexual activity, is affected by testosterone levels and medications as well as by the normal anatomy of the prostate and bladder. Decreasing amounts of testosterone, often occurring as a result of normal aging, will affect the volume of the ejaculate. Certain medications may also affect ejaculation. With aging, the volume of the ejaculate decreases.
– Surgery on the prostate or bladder and radiation can affect the amount of secretion produced as well as the ability to have normal ejaculation.
– Orgasm occurs as an experience of intense physical and emotional pleasure during the sexual act, and can occur separately and independently from erections, emission or ejaculation. Many factors, including emotional and psychological considerations, contribute to the experience of orgasm.
It is important to realize that male sexual function is defined by more than just the ability to have an erection. Mutually satisfactory sexual relationships can be maintained in the presence of impotence.
Chronic disease includes other cancer, hypertension, cardiac disease, diabetes or stroke.
Risk factors include antidepressant use, consumption of more than two alcoholic drinks per day, smoking, obesity, lack of exercise and watching television for more than 8.5 hours per week.
Impotence and Cancer Surgery or Radiation
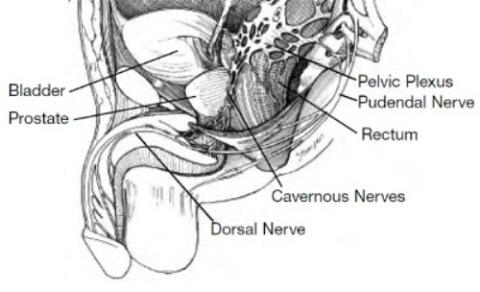
Impotence following major pelvic surgery or radiation, including prostate and bladder surgery, has been widely reported. During a radical prostatectomy the nerves which allow erection, called cavernous nerve bundles, and which lie within millimeters behind and on the side of the prostatic capsule, may be injured by being cut or separated from the prostate. This may cause temporary or permanent impotence, although sexual desire and the ability to achieve orgasm should remain. As discussed in Chapter Five: Other Causes of Impotence, radiation to the prostate, the bladder or rectum can damage the cavernous nerves as well.
The “nerve-sparing” radical prostatectomy or radical cysto-prostatectomy procedures to remove a cancerous prostate or bladder attempts to preserve these cavernous nerve bundles without compromising complete cancer removal. In the hands of an experienced surgeon, if both nerve bundles are spared, 50 to 90 percent of patients — depending on age and health — may have an eventual return of unassisted erectile function over time. When only one nerve bundle is spared, the percentage of patients that have return of erections over time is 25 to 50 percent. If a non-nerve sparing technique is used, the potency rate drops to 16 percent or less, depending on patient age.
Aside from the degree of nerve-sparing surgery performed, other factors are associated with impotence after radical prostatectomy.
- The biggest risk factor is age. Studies have shown that while the majority of men under 50 years of age are potent after radical prostatectomy, only 22 percent of men over the age of 70 are potent after the procedure.
- Other medical conditions that increase the risk of impotence include hypertension, smoking, diabetes, elevated cholesterol (hyperlipidemia) and heart disease. Depression, as well as other psychogenic factors, may affect psychological well being and recovery of potency.
- Unfavorable clinical and pathological stage of cancer also is associated with worse potency outcomes, as these men may not be candidates for a nerve-sparing approach because it may leave cancer behind.
It should be remembered that even if both nerve bundles are spared, with their proximity to the prostate (See Figure), these structures will likely suffer some injury that will take time to heal. Healing of the cavernous nerves and return of any unassisted sexual function may not begin until six months or more after surgery; however, it usually continues to improve over the next two to three years. Indeed a large percentage of men may not recover sufficient function for 18 to 24 months, some even longer. With prolonged disuse, the smooth muscles of the penis may atrophy, which worsens erections. Early and aggressive treatment of impotence with oral or injection medication may improve and speed up recovery of erectile function.
For men undergoing radiation, the amount and extent of radiation as well as whether or not they are treated with hormone therapy correlates with the likelihood of impotence, either temporary or permanent. The reduction in libido and possible difficulties with erections from the use of hormone therapy is generally reversible when the therapy is discontinued. The likelihood of irreversible effects is related to patient age, pre-treatment sexual function and the length of time hormone therapy is given.
Even if impotence is present after surgery or radiation alone, the ability to achieve an orgasm should remain. However, with the prostate removed there is no ejaculate although some secretions may remain. During orgasm, there is no emission or expulsion of semen. The ejaculate volume will decrease with radiation as well.